Well, not for the moment, at least. But watch out.
I didn't have time to go for my camera before this moment disappeared, so I settled for this with my phone.Thursday, April 12, 2007
Saturday, April 07, 2007
Probably Free to a Good Home
(20th & College on Beacon Hill)
Paternity leave, Day number I'm not sure anymore. It's not such a lovely day today as it was the last two (70s-80s, sunny, mountains out...), but still the outside was inviting, so after two cups of strong drip coffee I strapped Elliott to my chest, put a leash on Yagi, and headed out for a walk around Beacon Hill. Our destination was, bien sur, Galaxie, but the route was to be improvised. I've not yet walked through that neighborhood, and was quite pleased with the sights. There are great views of the mountains and across the valley to the Mount Baker neighborhood. The housing in dense and old, mostly. Lots of old craftsman homes from the 1920s, many are well-maintained, but there are a few that need some love. There are also a bunch that qualify as tear-downs.
We wound our way up the hill, following interesting sights and quiet streets on our way to the coffee shop. I spoke with my mom for a while while we walked, and she told me of her afternoon yesterday with Zoë, who is visiting St. Louis with Brooke this week.Galaxie was packed. I hooked up Yagi out back next to a woman eating her breakfast. He begged until she gave him a piece of sausage. I got coffee--it takes me two at home plus a double-shot latte to get to "normal" these days--and talked with Woody a little about the benefit they're having tonight--wheelchairs for someplace in South America. Galaxie would be a great place for a party (and has a liquor license, which helps), but I'm not looking for a place to host anything these days.
Coffee was to go today, and we set out down the hill by a new route, admiring the sights and looking for the worst houses on great blocks, a buying strategy I'm obsessed with lately, though it will be another fifteen months or so before we're looking for anything. And who knows where we'll be looking?
It rained lightly as we neared the bottom of Beacon and entered the roaring Rainier Valley. It felt nice, the rain, and I let the drops fall on Elliott's head so she could appreciate them too.
We were out about an hour and a half, home just in time to feed Elliott and beat the heavier rain. Now all the critters are asleep but me. I would be too if I were smart, but I'm glad I stole a few minutes to write about our morning.
Wednesday, April 04, 2007
I love spring in Seattle
Sunday, March 18, 2007
Friday, March 16, 2007
Movin' On Up
Algorithmanic episodes
 Jerome Groopman has been all over NPR the last few days giving interviews about his new book, How Doctors Think. This morning he landed a seven-minute session on Morning Edition, and recently spoke at length with Terry Gross on Fresh Air. The book sounds like a well-constructed inquiry into the algorithmic processes of doctor think. How do physicians make sense of patients' stories and arrive at a diagnosis?
Jerome Groopman has been all over NPR the last few days giving interviews about his new book, How Doctors Think. This morning he landed a seven-minute session on Morning Edition, and recently spoke at length with Terry Gross on Fresh Air. The book sounds like a well-constructed inquiry into the algorithmic processes of doctor think. How do physicians make sense of patients' stories and arrive at a diagnosis?Or a mis-diagnosis. Groopman discusses the experiences of physicians and patients--even his own experience as a patient, to point out where doctor think goes wrong. The diagnostic process, relies on information from the patient about symptoms, personal and family history, risk factors. Doctors then collect relevant "objective" data (physical exam, labs, studies), and assemble a list, or differential diagnosis we think might explain what the patient is experiencing. Ideally, it's an exhaustive list, and we narrow it with directed studies to rule things in or rule them out. We work hard at it, but for various reasons we don't always get it right, and the consequences can be severe. Dr. Groopman explains to Steve Inskeep on Morning Edition:
An anchoring mistake? Sounds like what my people call early closure, a very common"Usually doctors are right, but conservatively about 15 percent of all people are misdiagnosed. Some experts think it's as high as 20 to 25 percent. And in half of those cases, there is serious injury or even death to the patient."
Why do you think that doctors would be wrong that often?
Well, you know, it's very hard to be a doctor. We're working under tremendous time pressure, especially in the current medical system. But the reasons we are wrong are not related to technical mistakes, like someone putting the wrong name on an X-ray or mixing up a blood specimen in the lab. Nor is it really ignorance about what the actual disease is. We make misdiagnoses because we make errors in thinking.
We use shortcuts. Most doctors, within the first 18 seconds of seeing a patient, will interrupt him telling his story and also generate an idea in his mind [of] what's wrong. And too often, we make what's called an anchoring mistake — we fix on that snap judgment.
 problem. Making big differentials is hard, and many things influence how quickly we decide we know the diagnosis. Often, it just seems to fit...mostly...more than other stuff. But is our list comprehensive? Did we consider only common diagnoses? Is is time to trot out the rare, eponymous syndromes we memorized in med school but have never seen? Deciding early to attach a diagnosis to a symptom feels good, especially when there are other patients with symptoms waiting to be seen.
problem. Making big differentials is hard, and many things influence how quickly we decide we know the diagnosis. Often, it just seems to fit...mostly...more than other stuff. But is our list comprehensive? Did we consider only common diagnoses? Is is time to trot out the rare, eponymous syndromes we memorized in med school but have never seen? Deciding early to attach a diagnosis to a symptom feels good, especially when there are other patients with symptoms waiting to be seen.There's something about categorization that appeals to me. Calling something anchoring mistake, when you could just as easily call it laziness, gives me a kind of hope. If I miss a diagnosis and because I'm lazy and the remedy is to "try harder," well, I'm screwed. The problem and the solution are both pretty vague, and my fear around messing up again takes over. Fear motivates, for sure, but I would argue the outcomes aren't so great.
If I can categorize my apparent laziness with nifty terms like anchoring mistake (in which I make a snap judgement) or representativeness error (wherein I tell myself that common things occur commonly), my type-A doctor mind has something productive and familiar to do: memorize a list. In this case, knowing the ways my thinking might not serve me well helps me see potential pitfalls in diagnosing and treating--also known as helping--patients.
I haven't read the book yet, but I will. I did, however read Dr. Groopman's article from January 29, 2007 in the New Yorker. The writing is excellent and the examples compelling. If the book is anything like the article, I'll be reading all weekend.
Match Day
"The Match" -- a high-anxiety cap to the end of a grueling four-year medical education -- will determine their professional futures, not just where they will live for the next three to seven years, but what specialty they will pursue.Well, that all sounds quite difficult, doesn't it? True, medical training isn't easy, but it's not Darfur. There's a language tossed around in the press that creates this mystique of systematic torture by drill-sergeant faculty.
There's a buzz going on, but the excitement has the tamped-down quality of people who have learned to manage anxiety to survive the rigors of clinical rotations, being called out for not knowing answers during rounds and monster exams.
There is recognition, too, that as hard as medical school was, residencies, renowned for their brutal on-call schedules, can be even harder.
The UWSOM event is quite informal: lots of milling about, tamping down anxiety and eating dry pastries until the envelopes are distributed. You can open your envelope when you want and with whom you want. Some schools parade students in front of a crowd to read their "fate" for everyone. Check out this video from yesterday's University of Cincinnati Match Day event.
I would rather die than participate in that. Sorry, Shannah.
On the residency end, we go about our business on the morning of The Match and wait for a mid-morning page with the list. I got the page as I was strolling home from my massage through a sunny Seattle park. Quite a different scene than in Cincinnati or even at here at UW. I was thrilled with how we matched overall and especially at my beloved Downtown Public Health clinic.
Back to my brutal schedule--last legitimate day of vacation.
Thursday, March 15, 2007
What the fe-mail-man brought
March in Seattle
Out walking this morning I tried to capture these brilliant yellow blooms with my low-res camera phone. Not too impressive, but also gives me an opportunity to figure out how to post directly from my phone.
More vacation
Yesterday there were a couple of things on the list that I felt I had to do. We got rid of Brooke's desk the other day--gave it to Hilary and Dan for their new house--to free some space for a crib, glider, and changing table Brooke picked up on craigslist. Those things go into the current guestroom, soon to be Elliott's room. The desk is gone, and all the stuff that had been in the desk was on the floor, waiting for me to sort through it. What a lot of junk: about 75% of it went straight out the door, either to the garbage or to Goodwill. There is still some stuff there that I couldn't part with (but should). I created a defer decision pile and made some lame excuse to Brooke for why I couldn't deal with it that moment. She didn't buy it, but she didn't call me on it, either. So there it sits. Overall, I did not enjoy that chore.
Next on the list was to return a bed to Ikea. Brand new and yet-unassembled (but out of the box), we slogged it down to Southcenter (big box retail hell) to get it out of Elliott's room. That was the second unused new bed we unloaded this week. Ikea gave us store credit, since we were beyond the return period and didn't have a receipt. We walked around the store for a while and found some more crap to bring home to replace the stuff we spent the morning purging. New crap, though; the other stuff was old crap.
On the way home the first thing we did was get lost. Happens every time we go to Big Box Hell. After a slow tour of the Valley Medical Center parking lot, we inched onto the freeway and
 eventually onto the I-405 HOV lane, which moved at about 60mph while the other three lanes literally sat still. Traffic was miserable all over due to accidents and a big police foo-faa over a stolen car.
eventually onto the I-405 HOV lane, which moved at about 60mph while the other three lanes literally sat still. Traffic was miserable all over due to accidents and a big police foo-faa over a stolen car.I hate car life. I would prefer to walk or bike or bus or run everywhere I need to go. But...but...you know I'd like to say now "that's just not practical." But...it IS practical. As Bus Chick points out every day, we've got great public transit. I could easily take Zoë around town on my bike, and the trip from here to daycare and work is all on trails or wide, dedicated bike lanes. And I've demonstrated to myself that running is feasible, having commuted that way nearly all of last year. But then I got a car. Terrible idea! Immediately I started driving, taking advantage of the free parking I have at work and the ease of just getting in and going. I've paid the price with ten pounds gained and physical fitness lost. If I can park a car at work, I can also park a jogging stroller.
Just takes a little planning, which will be easier when I'm not so sleepy all the time. Any day now, I'm sure Elliott will just sleep right through the night. Any day.
Tuesday, March 13, 2007
Vacation
 I'm off work this week. It's good. We thought about going away for a few days, renting a cottage on Whidbey Island or Hood Canal. That would be good fun, if it weren't for Zoë and Elliott and their dueling sleep schedules...well, their awake schedules, I should say. It's bloody exhausting. Weekends turn out to be pretty hard, and three days in a cottage, even in a lovely setting and even with a hot tub, would have been less like a vacation than like work. The alternative was to stay in Seattle, send Zoë off to day care in the morning, and enjoy life with one very portable infant. We can take naps, write, go for walks, get massages, all thanks to the happy two-parent-to-one-child ratio we used to think was so hard. Yesterday we called Sam to babysit for the afternoon, then headed out for lunch at High Spot and a walk. No nap.
I'm off work this week. It's good. We thought about going away for a few days, renting a cottage on Whidbey Island or Hood Canal. That would be good fun, if it weren't for Zoë and Elliott and their dueling sleep schedules...well, their awake schedules, I should say. It's bloody exhausting. Weekends turn out to be pretty hard, and three days in a cottage, even in a lovely setting and even with a hot tub, would have been less like a vacation than like work. The alternative was to stay in Seattle, send Zoë off to day care in the morning, and enjoy life with one very portable infant. We can take naps, write, go for walks, get massages, all thanks to the happy two-parent-to-one-child ratio we used to think was so hard. Yesterday we called Sam to babysit for the afternoon, then headed out for lunch at High Spot and a walk. No nap.Last night, we gave Elliott a bath, which I videotaped and and
 might post if Brooke can get over thinking our children will end up like the Star Wars kid or that poor Numa Numa Dance fellow. I don't see it happening with the bath video, but maybe with Zoë's "Shake Your Booty" song.
might post if Brooke can get over thinking our children will end up like the Star Wars kid or that poor Numa Numa Dance fellow. I don't see it happening with the bath video, but maybe with Zoë's "Shake Your Booty" song.Also last night we completed season five of 24. I love the series, and season five was great, especially Gregory Itzin and Jean Smart as the president and first lady. I've now seen the whole thing through last season, and haven't a clue what has happened this season. I'm pretty sad to read that Melanie McFarland, the most trusted hairdo in TV reviewing, isn't "feeling it anymore." It will be a while before I can start in on season six. What'll we watch next? Back to Entourage, perhaps, so I can dream of being a movie star.
This morning I got in a good long walk with Yagi. Through the I-90 walking tunnel, down to the lake, and along the water while Yagi swam and carried big sticks. I'm off now for a haircut, then to pick up Zoë. Again, no nap. What the hell is going on here?
It's a nice pace. Next time maybe we'll go for the cottage.
Patient Satisfaction
 usually following publication of research or polls. I'm interested in what contributes to satisfaction in the patient-doctor relationship, though I'm not convinced that we need to be satisfied to have our needs met. Or, put another way, offering the best and safest medical care may not always satisfy my patients--or me. There is a lot of research about satisfaction, but no clear evidence that satisfaction matters. It is assumed to be its own valid outcome, though it is hard to measure reliably. There are a couple of fun satisfaction items that have landed in my Google Reader recently.
usually following publication of research or polls. I'm interested in what contributes to satisfaction in the patient-doctor relationship, though I'm not convinced that we need to be satisfied to have our needs met. Or, put another way, offering the best and safest medical care may not always satisfy my patients--or me. There is a lot of research about satisfaction, but no clear evidence that satisfaction matters. It is assumed to be its own valid outcome, though it is hard to measure reliably. There are a couple of fun satisfaction items that have landed in my Google Reader recently.Yesterday I ran into this Annals of Internal Medicine study on management of patient expectations. The investigators audiotaped 200 medical visits and documented what patients wanted, then asked them later how they felt about the visit. It turns out that 97.3% of pre-visit expectations were at least discussed during the visit. How did these expectations come up? Forty percent of the time patients brought up directly ("I would like _______." Good, solid communication). Thirty percent of expectations came out by having patients mention symptoms. Also good communication; it's my job as a doctor to help people make sense of their symptoms. More than a quarter of expectations came out through "physician-initiated discusson." I'm not sure exactly what that means. Would patients never have mentioned these things if the doctor hadn't chased after it? Or did the doc just get there first? Thinking about this would get me way off track, so I'll drop it.
Regardless of how things came up, expectations were met around 67% of the time, and where doctors weren't comfortable, they did the right thing and suggested alternatives only around 22% of the time. I guess the rest of the time they just said: "Uh, no."
 And what about satisfaction? "Patient satisfaction and trust remained high, regardless of whether expectations were met." So what can I learn from this study? Should I worry about what patients expect? If expectations aren't related to satisfaction, well then what is? And does satisfaction matter? I know plenty of people who aren't satisfied with their doctors, but they keep going.
And what about satisfaction? "Patient satisfaction and trust remained high, regardless of whether expectations were met." So what can I learn from this study? Should I worry about what patients expect? If expectations aren't related to satisfaction, well then what is? And does satisfaction matter? I know plenty of people who aren't satisfied with their doctors, but they keep going.Item number two showed up in Family Practice Management's March News & Trends, reporting on a Consumer Reports survey. I've pasted the clip in green below with my comments along the way.
The good news for physicians: The overwhelming majority of patients said they were "highly satisfied" with their doctor and that their health improved under their doctors' care. In addition, 77 percent said their doctors treated them with respect and 67 percent said they were patiently listened to and understood.
Already this seems more useful than the Annals piece, as they ask whether patient health actually improved. I'm also happy CR asked about respect, but shocked that so few doctors listen to and respect their patients. CR presents this under the good news header!
The bad news for physicians: The majority of patients said their doctors never talked to them about the cost of treatments and tests.
I hate talking money with patients, and frankly feel ill-equipped to do it. I know tons about tests and treatments, but very little about what they cost. My ePocrates handheld reference gives me some info, but I can't predict what insurance will cover and at what rate. I saw a patient in clinic one day with chest pain. It wasn't his heart, but when I shared with him some chest pain (i.e. heart attack) warning signs that should prompt him to call 911, he began to quiz me on on the costs of ambulance transport and emergency care. I had no idea what to tell him, and felt bad about it. I know money matters, but I just don't have the answers.
In addition, patients had these complaints:
• 74 percent said their physicians had not asked about emotional stress.
• 24 percent said their physicians made them wait 30 minutes or more.
• 19 percent said they couldn't get an appointment within less than a week.
 I cannot believe that there are still non-surgeon physicians who don't ask about stress. The second two complaints above are systems issues, and inexcusable. I think making patients wait around to see a doctor demonstrates a real lack of respect for the value of their time. Patients don't have all day to hang out in clinics, waiting to be seen. Also, having to wait a week when you're sick or when your kid is sick and you're worried is just plain wrong. Who wouldn't go to the ER under those circumstances? Same day or next day access isn't that hard to provide; we should be doing it.
I cannot believe that there are still non-surgeon physicians who don't ask about stress. The second two complaints above are systems issues, and inexcusable. I think making patients wait around to see a doctor demonstrates a real lack of respect for the value of their time. Patients don't have all day to hang out in clinics, waiting to be seen. Also, having to wait a week when you're sick or when your kid is sick and you're worried is just plain wrong. Who wouldn't go to the ER under those circumstances? Same day or next day access isn't that hard to provide; we should be doing it.
Sure. But I haven't done my back exercises in months, so I get that it's not always easy to do what you're told, even when you know it will help.
Other physician gripes included the following:
• 41 percent said that patients wait too long before making an appointment.
Or are they just waiting for their appointment?
• 32 percent said patients are too reluctant to talk about their symptoms.
Except emotional stress, which we don't want to talk about.
• 31 percent said patients request unnecessary tests.
Bloody internet.
• 28 percent said patients request unnecessary prescriptions.
Bloody advertising. In this case, I refer back to the Annals paper, which reminds us that it is important to negotiate with patients. We shouldn't offer wasteful or harmful interventions to patients, even if they want them. We should offer alternatives that address patient concerns and hopes.Two more publications on satisfaction, and I still have no good idea about it's value, or even what it really is. I do know there is value in listening and respecting patients, getting them in when they need me and seeing them on time. And I'd like them to feel healthier.
But satisfied?
Sunday, March 11, 2007
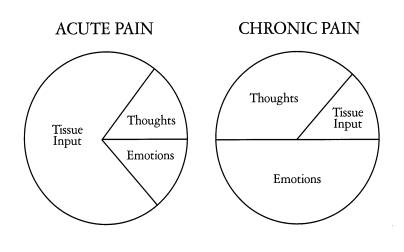
Pain on the Brain
 Recently, my residency program has been working on how we help patients with pain. Honestly, some of this comes from the great frustration the doctors and staff at our three clinics feel with "pain patients." It feels like patients with chronic pain take up a lot of our time and energy, and we end up not helping them very much--they still have pain. Stuck in our doctor brains is the notion that if something is wrong, we should be able to fix it, or at least help patients fix it. So when things don't get better--the pain is the same or worse--over months of treatment, we get frustrated, and so do our patients.
Recently, my residency program has been working on how we help patients with pain. Honestly, some of this comes from the great frustration the doctors and staff at our three clinics feel with "pain patients." It feels like patients with chronic pain take up a lot of our time and energy, and we end up not helping them very much--they still have pain. Stuck in our doctor brains is the notion that if something is wrong, we should be able to fix it, or at least help patients fix it. So when things don't get better--the pain is the same or worse--over months of treatment, we get frustrated, and so do our patients.One of the most difficult issues revolves around pain medications, specifically narcotics. Treatment of chronic pain with opioids (commonly vicodin, percocet, oxycodone, and methadone in our clinics) has a long history, and opinion about its value and safety seems to swing like a pendulum. In primary care settings, the pendulum has swung into the "avoid narcotics" zone over the last several years. There is a lot of well-founded concern for the long-term safety of narcotics, and for the harm we do to patients by creating dependence on these medications. But that's not what really makes us uncomfortable.

It's a trust thing. Misuse of narcotics--overuse, diversion--is a reality, and doctors are justifiably nervous about the possibility that the potent medications we prescribe might be used to feed addiction or for monetary gain. There's good evidence that this happens, even among patients we believe to be using narcotics appropriately. We can't be sure, and we're not comfortable with a sham therapeutic relationship.
Unfortunately, that anxiety about trust sets up a difficult relationship with patients when they come to us with pain. When I hear a patient report low-back pain, my differential diagnosis always includes inappropriate drug-seeking behavior. There is no other complaint that sets off these kinds of alarms. I find that when this suspicion come up, I might test a patient with a few non-narcotic suggestions, like physical therapy, but these maneuvers only contribute to the discomfort and don't clarify anything. Worse, failure to embrace physical therapy as the best idea ever and suggest, perhaps, a short course of vicodin ("I had some left from a procedure and they seemed to help") puts the patient at risk of being branded as a drug seeker--the pseudo-addict.
All of this has been stuck in my sleepy head recently as I've done this narco-dance with a few new patients and worried a lot about how to wean the few patients of mine who take opiates chronically. The residency pain task force is doing it's thing, and will certainly produce some helpful resources for my patients, but I'm not good at waiting, and the folks I care for have pain now.
 A couple of weeks ago I put together a five page "Menu of Treatments for Low-Back Pain" for one of my patients. I had hoped to use some chronic disease management techniques to create a plan with her that would be as transparent as possible. I created the menu from the collected works of the Cochrane Back Group and offered it to her as a way to start us both thinking about how to help her to a tolerable level of pain. The menu concept is popular in managing chronic diseases like diabetes and hypertension that require patients to change behaviors. It gives people options and lets them choose what they think they can do. It is important to build the menu around goals--another chronic care pillar--and so we spent some time discussing what she hoped to accomplish regarding her pain. I thought it went well.
A couple of weeks ago I put together a five page "Menu of Treatments for Low-Back Pain" for one of my patients. I had hoped to use some chronic disease management techniques to create a plan with her that would be as transparent as possible. I created the menu from the collected works of the Cochrane Back Group and offered it to her as a way to start us both thinking about how to help her to a tolerable level of pain. The menu concept is popular in managing chronic diseases like diabetes and hypertension that require patients to change behaviors. It gives people options and lets them choose what they think they can do. It is important to build the menu around goals--another chronic care pillar--and so we spent some time discussing what she hoped to accomplish regarding her pain. I thought it went well.Mind you, in several visits we haven't touched on her hypertension, diabetes, or hyperlipidemia. And I haven't gotten close to talking about preventive care: pap smears, osteoporosis, etc. Missing these things is another hazard of chronic pain.
Okay, so I started this not to whine but to describe a chain of events and some hopeful developments. The back pain menu was a nice little organizing moment for me. There are heaps of options for patients with pain. For any given intervention, the data might not be thrillingly positive, but most of them work for somebody, and in combination, I have to believe that we can find a way to decrease pain.
We've also got resources in our own clinics. Like chronic disease management techniques, cognitive behavioral therapy techniques have a place in the management of chronic pain: one's process of thinking-feeling-behaving is vital to one's experience of pain.
As an exercise in organizing these ideas into a practical approach, I'm working on a web-based collection of resources. The Pain Page will catalog evidence-based interventions for pain, local resources, patient perspectives on living with pain, media coverage of related issues, and how our work as physicians and patients relates to regulatory bodies.
I hope this will help my colleagues, patients, and me build together a transparent and effective structure for collaborating on a problem we all would like to handle better.
Sunday, February 25, 2007
Galaxie
And then yesterday, out of nowhere, this great experience came up. The four of us headed out on Saturday morning to the Galaxie café, a Beacon Hill coffee shop opened recently by our neighbors, Yen and Jeff. The place is great! It was quite lively, good coffee, pastries. The sandwich menu looked fantastic. But don't take my word for it, read the P-I review. There were also a bunch of kids there, and Zoë had a great time with the other kids and toys.
The interior walls are decorated in Beacon Hill murals, and the entire south wall is a building-by-building map of the neighborhood. Local customers can put a pin in their house--and there are quite a few pins. We called our friends, Sachi and Travis, to walk down and join us. They did, but I don't think they put a pin up. Next time, perhaps.
Best of all, it was a chance to do something social--in public--as a family. Brooke and I never really got to hang out in cafes much together before we had kids, which I kind of regretted. Now we can. And we'll be back there next weekend.
Saturday, February 24, 2007
OB-RAMA part II: Noon - 5am
Maybe a mistake, looking back.
I discovered that I was to be "paired" with one of the interns who is also a medical school acquaintance of mine. Let's call her Tatum, which happens to be her name. I wasn't thrilled about being teamed up with Tatum, or with the idea of "shadowing" an intern at all. I've been an intern, completed my internship, and enjoy the rhythm and responsibility of my second year much more. Interns have crappy hours and few choices. Surgery interns have horrendous hours and buckets of scut packaged in an oppressive hierarchy. It's not my world. I'm okay visiting for a bit, but not so much with Tatum as my guide. But what can you do?
I got a brief explanation of the team structure from Tatum and an offer to go to the OR to scrub for a case. I declined, thinking I'd rather spend time learning about the patients on service. I'm also just not that interested in hanging out in the OR holding retractors. Instead, I familiarized myself with the in-house patients, returned to my postpartum mom & babe duo, and did some paperwork. Tatum and I had divided up her patients among us for the morning--I was to see half of them (about six) before 7am.
At about 4:30pm Brooke called to see if I could pick up Zoë from daycare on my way home. I said yes and made one last call to clinic to check in. Our nurse there told me that another of my pregnant patients was having contractions and was on her way in. It doesn't take long to assess whether a woman in active labor and needs to be admitted, so I walked up to OB Triage to wait for her. Annabella (not her name, but the surgery intern is definitely named Tatum for real) arrived a few minutes before 5pm. She was still shy of getting a room by my evaluation, but I thought she would be in active labor after a couple of hours of walking, so I sent her out and picked up Zoë as planned, knowing I'd be back shortly.
My colleague Sharon examined Annabella when she returned, determined she was "active" and got her a room. I was back before 8pm, and based on my exam, I calculated that she might deliver at about 2am. I'd be there until 3am, at least, and had clinic the following afternoon, which I don't like to cancel. Based on that, I figured I should do something about the morning (rounds and retractor holding), which might be my only chance to sleep, keeping in mind that at 7am I'd be over my duty hours for patient care, with at least ten hours of care still scheduled.
As an R2, I have a variety of responsibilities and frequently have to prioritize them in unfortunate ways. Occasionally clinic gets canceled due to a delivery. Everything can get canceled if I'm "goated" to fill in for a colleague who is unable to work. In this case, I was looking at three responsibilities, a duty hour conflict, and no sleep for nearly 40 hours. It didn't take long to figure out that if something was going to go, it would be "shadowing" a surgery intern for the morning and doing half her scut. Even if it were an intern I wanted to hang out with, I'd have made the same choice.
Here's what I did. I paged Tatum at home to let her know that I'd be up all night with a delivery and wasn't planning to see her patients in the morning--apologies. No skin off her nose, I figured: she'd be rounding on those patients if I weren't "shadowing." Shortly after I sent my text page, Tatum paged me back with a number. I called, and spent the next fifteen minutes listening to poor Tatum go on about my priorities and my work ethic, asking me what I intended to get out of my GenSurg rotation and grilling me on where I'd been all day.
Was she fucking kidding?
She wasn't. I'm not one to pull rank on anyone, it's not really what my people do (my people are family doctors, not surgeons). But holy shit! I couldn't believe this intern was giving me the third degree about my work ethic. I was at work. She was home eating pudding pops for all I know. After several minutes of actually indulging her line of questioning, I stopped and said, "Tatum, why are you giving me a hard time about this? Have I created some new work for you?" No! She's frickin' lazy and was pissed that she wouldn't have me around to do half her work for her. Argh.
That got me pretty riled, and I stayed that way for a while. I got it together for the delivery, though, which didn't happen until after 3am. Like the delivery the morning prior, it required a vacuum, but unlike that one, I figured out the vacuum myself. One pop-off and then a smooth delivery on vacuum attempt #2. Minimal tearing. Healthy mom and a healthy baby: that's pretty much my whole job.
I was done with the post-partum paperwork at 4am, and was on my way home when I decided that I would make one gesture to Tatum and anyone else on the surgery team that would call me weak and lazy for cutting out on a morning of doing someone else's busywork. I rounded on the damn patients from 4-5am, wrote notes, and sent Tatum a dawn page letting her know I'd done some of her work and that she should not ever put us through such an annoying conversation again.
That was 5am, which brings me to the end of the story, basically. The rest is pretty boring. I slept some, rounded on my moms and babes in the hospital, and spent the afternoon in clinic. It's now Saturday night and I'm off until Monday, when I'm back on the General Surgery team and will either face a hostile crowd (for being lazy & weak)...or no one will have noticed my absence.
OB-RAMA: Thursday, 4:30am - Noon
I woke up, sort of, on Thursday morning to my pager doing the single-beep-and-vibrate thing at about 4:30am. It was my colleague, Jessica, holding down the inpatient service on nights (I was on the week before). She had one of my two post-dates patients in triage, in labor and in pain. She was moving over to a delivery room. I told her I was on my way, but that I'd be moving slowly. And I did. Move slowly. I think I fell back to sleep for a bit, then got in the shower, tossed on some green scrubs, and headed out. I felt a little bit guilty leaving Brooke to wrangle both Zoë and Elliott, but what could I do? It's my job.
My patient, let's call her Frances, was dilated to 8cm when I arrived at the hospital, but the baby was still high in her pelvis. She had an epidural block, so she was comfortable, but neither she nor her husband could really rest, for they were both nervous and excited about what was happening. I got a little nervous too when I saw the fetal heart tone strip, which showed some prolonged rate decelerations, indicating that the umbilical cord was being compressed with each contraction. Decels themselves aren't alarming, and the cord compression variety are fairly benign, but these things were going on for longer than I would like. I chatted with my attending, Jay, about my options for managing this situation. He reminded me that in general there aren't that many options for managing labor, which is both a blessing (fewer decision to make) and a curse (in medicine it's nice to have options). The basic choices here were to start an amnioinfusion (put some saline into the uterus to create a bigger pocket of fluid around the baby) or do nothing. Amnioinfusion is one of those interventions that the evidence says doesn't do a whole lot of good in most situations but is fairly harmless. If these were actually cord compressions, it should help. So why not try, right? I also took a moment to curbside an obstetrician, who helped me feel better about infusing.
It helped! She labored on with a happier strip and eventually got to full dilation (10cm) and the baby descended nicely. Time to push, which she did, with coaching, for about an hour before the decels came back. Again, not terribly alarming, but we thought we'd feel better if we could just deliver this baby into the world and free her from being compressed every two minutes--clearly she did not dig the squeeze. Jay and I talked about a vacuum assist and got the OB involved to help with placement, as the baby's head was still a little high. A novice with the vacuum, I got two attempts (or "pop-offs"), then, by previous agreement) handed the vacuum over to more experienced hands. Frances pushed and we pulled and out came a lovely baby, who immediately enjoyed the change in atmospheric pressure. With nearly all vacuum-assisted deliveries, there is some tearing of maternal tissues, and this was no exception. A few stitches and that was that.
Then of course, paperwork. A delivery note, post-partum orders for mom, a newborn exam, note, and orders and the odd surveys, code status declarations, and face-sheet (billing) stuff that litters the chart.
It was noon when I finished that, and this post is long enough, so the day will continue under another post.
Friday, February 16, 2007
Status-post
I took advantage of the hospital network's streaming video access and checked in nightly on both the Daily Show and Colbert Report. Last night I jumped from Comedy Central to ABC and watch the last two episodes of Lost, which look pretty good online, the non-skippable ads notwithstanding.
Every space needs ambiance, right? I dig the new lighting in the Gumby Lounge and each night killed the overhead fluorescents in favor of mellow area lights. Greg Parker clued me in to Soma FM a few nights ago, and the selections there became the background of the space for the duration of the week. Not so much an office but a working lounge. Many thanks to Anneliese and Sarah for the improvements!
I did spend one night on my own due to Maria's illness. Far from being a burden, it was actually quite fun. I took advantage of my solo-status to (a) feel confident in my medical decision making and (b) look up everything. Many thanks to UpToDate and my trial of ePocrates expanded version for helping with differentials and treatment options.
Thanks to my colleagues on the service and around the hospital for making the week fun, too!
Now for the return to daytimes. This is the worst part--several days of sleepy, surly confusion. Fortunately, it's a long weekend, and being alert at night can actually help Brooke get some sleep--I'll cover some of the nighttime attention Elliott needs.
Friday, February 09, 2007
Bloomin' Seattle
 Inspired by a recent post by Bus Chick, I snapped this (phone camera) shot a few minutes ago near my house in the Rainier Valley. I saw lots of tiny blooms on my walk to and from Dahlia Spa. Seeing new blooms in Seattle means that it must be February. The days are finally getting a little longer, and soon we'll all be making vitamin D again. It turns out to be just about the nicest day in recent memory here: thin cloud-cover and a mild 57-degrees as I write.
Inspired by a recent post by Bus Chick, I snapped this (phone camera) shot a few minutes ago near my house in the Rainier Valley. I saw lots of tiny blooms on my walk to and from Dahlia Spa. Seeing new blooms in Seattle means that it must be February. The days are finally getting a little longer, and soon we'll all be making vitamin D again. It turns out to be just about the nicest day in recent memory here: thin cloud-cover and a mild 57-degrees as I write.Tonight I begin a week of night shifts on the SFM inpatient service. The transition into nights is always tough, but easier than returning to days. No one much enjoys my cross attitude during the days that follow night float. Fortunately for my family, it doesn't happen that often.
If I'm lucky, I'll get some good posts in over the next several nights. A hospital at night is a strange and wonderful place--so is the company one keeps. More from the other side.
Monday, February 05, 2007
Gellin'

Hand gel has been all over the news recently. Last week a study appeared discussing hand sanitizer technique--apparently it matters (I'm looking for that link). A bit appeared this weekend about the growing recreational use of alcohol-based gels in prisons (my search for Purell Appletini actually yielded something). And there's a new nicotine hand gel on the market (PubMed searches reveal no research on the stuff).
Makes me wonder what can't be delivered with a little gel?





